What is Revenue Cycle Management Optimization?
Revenue Cycle Management (RCM) optimization is the process of improving how healthcare organizations handle patient billing, medical coding, claims management, and payment collections to maximize revenue and speed up reimbursements.
By addressing key issues early, like insurance eligibility verification, accurate charge capture, and clean claims submission, RCM optimization helps reduce claim denials, shorten payment cycles, and improve cash flow.
Through automation, data-driven performance metrics, and streamlined workflows, healthcare providers can lower their cost to collect, boost efficiency, and maintain compliance across the entire revenue cycle.
In short: RCM optimization helps healthcare organizations get paid faster, improve financial performance, and enhance patient satisfaction while ensuring compliance.
Table of Contents
Key Takeaways
- Revenue cycle management optimization fine-tunes each phase from patient access to final payment to drive the highest net revenue and eliminate waste. Calibrate workflows, technology, and roles to fuel accurate billing, clean claims, and fewer denials.
- Focus is on sustainable revenue growth and lower cost to collect while maintaining compliance. Align RCM objectives with your organizational priorities and unify workflows across squads.
- Revenue cycle optimization means financial performance with steadier cash flow, fewer errors and faster reimbursement. Track before and after metrics to prove gains and redirect resources to high-value care.
- Fortify operations with a rigorous playbook spanning pre-service, service capture, claims and billing, post-service resolution, and ongoing analytics. Set accountability, automate key tasks, and train staff.
- Use automation, AI, and predictive analytics to avoid denials, triage work, and predict cash flow. Guarantee interoperability across EHR, billing, and scheduling systems to preserve data integrity and compliance.
- Measure success with transparent KPIs that extend from foundational to advanced to predictive. Leverage real-time dashboards, daily checkpoints, and benchmarking to push proactive improvements and sustain results.
Revenue cycle management optimization is the organized enhancement of billing, coding, claims, and collections to increase net revenue and reduce days in accounts receivable.
It centers on front-end eligibility checks, precise charge capture, clean claim rates, denial prevention, and timely follow-up across payers. Teams leverage transparent KPIs, including first-pass acceptance, DNFB, and cost-to-collect, along with lean workflows that utilize rules engines and automation.
A short case view grounds it: a mid-size clinic cut AR by 12 days after fixing eligibility edits.
What is RCM Optimization?
RCM optimization is the work of increasing financial performance and velocity across every aspect of the healthcare revenue cycle, from initial patient registration to final patient payments. It streamlines workflows, tools, and roles of healthcare providers to eliminate waste, close revenue leaks, and ensure timely reimbursement. This process demands regular tuning as rules, payers, and patients’ needs shift.

The Core Definition
RCM optimization fine tunes every point in the cycle: patient access, eligibility and benefits checks, cost estimates, coding, charge capture, claims, payment posting, follow up, so billing is accurate the first time and cash flow is timely. It combines industry best practices, transparent workflow rules, and cutting-edge technology including eligibility APIs, claims scrubbing and rules engines.
The objective is clean claims, fewer denials, and less rework. Strong data management sits at the center: correct patient and payer data, standard code use, audit trails, and role-based access to protect privacy. Bad data is a leading source of denials, so front-end data quality checks and continuous data hygiene are fundamental, non-optional activities.
The Strategic Goal
The aim is to increase net revenue while reducing cost to collect and other frictions. Teams optimize intake, minimize manual keying, and employ automation where it delivers ROI, frequently resulting in 20 to 30 percent labor savings.
Faster estimates are a good sign: one group cut estimate time from five minutes to one, which raised price clarity, sped scheduling, and lowered bad debt. Cash flow benefits as well when days in accounts receivable drop and first-pass yield increases. Leaders monitor KPIs such as days in accounts receivable, denial rate, net collection rate, underpayment recovery, and patient satisfaction.
They fine-tune the program to payer shifts, fee schedules, and new compliance rules, all without interrupting daily work. RCM strategy has to align with the health system’s mission, which includes access, quality, and growth, and comply with privacy, security, and billing integrity standards. The plan needs to be straightforward, quantifiable, and designed for transformation.
The Financial Impact
| Metric | Before Optimization | After Optimization |
| Net revenue (USD) | $80,000,000 | $90,000,000 |
| Days in AR (days) | 55 | 38 |
| Denial rate (%) | 12 | 9 |
| Cost to collect (%) | 5.5 | |
| 4.2 |
Time to patient estimate (min) | 5 | 1 | Underpayments recovered (USD) | Limited | $10,300,000 (13%)
Cash flow stabilizes as denials decrease and first-pass clean claims increase. AI-powered edits and prediction can reduce denials by at least ten percent within six months, particularly by flagging patient data errors pre-submission.
Less rework, less write-offs, and faster payer responses is what fewer billing errors translate to. Automation eliminates low-value clicks, which reduces costs and liberates staff to manage complex cases and appeals.
Profitability increases as waste decreases and revenue leakage shuts. While many providers discover astonishing underpayments, one identified $10.3 million, or 13% of revenue. System-level inefficiencies continue to cost the sector billions annually. Rarely do we see the initial results of an RCM Optimization engagement hold.
How to Improve Revenue Cycle Management?
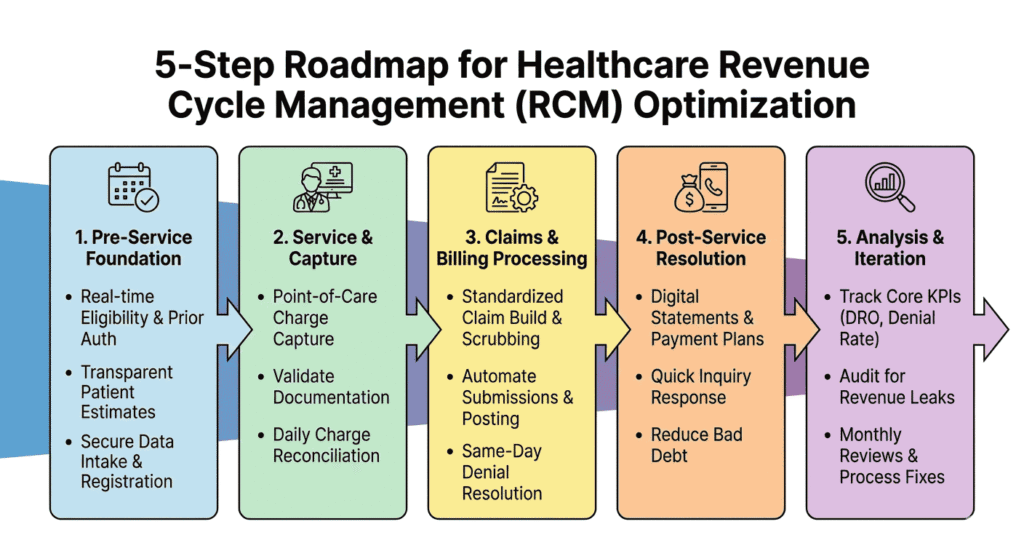
A robust healthcare revenue cycle links front-desk intake, clinical work, billing processes, and follow-up without leaks, aiming for clean data, clean claims, and fast cash.
- Map each step from scheduling to zero balance
- Assign owners, SLAs, and handoffs for every phase
- Standardize forms, codes, and payer rules
- Automate eligibility, coding edits, and claim scrubs
- Track KPIs daily; review trends weekly and monthly
- Train staff often; audit for accuracy and compliance
- Address denials within 24 to 72 hours. Apply a 21-day check.
- Offer digital tools for patients: estimates, pay plans, portals
1. Pre-Service Foundation
Get real-time eligibility and prior authorization checks at scheduling and registration. Capture legal name, date of birth, payer ID, and referral information accurately to reduce rework.
Provide transparent pre-service estimates and payment choices, as patients now foot around 22.9% of healthcare bills. Price transparency reduces sticker shock and increases point of service collection.
Cut no-shows with online booking, SMS or email reminders, and waitlists. Secure data intake with photo ID capture and insurance card scans to avoid downstream denials.
2. Service and Capture
Combine EHR and billing to automatically push charges, modifiers, and notes. Validate documentation at point of care so codes support medical necessity.
Train clinicians and coders to maintain coding throughput greater than 95 percent, meaning less than 5 percent stuck in queues. Missed charges flag, whether due to human error, technology gaps, or payer issues, run daily charge reconciliation to surface them.
Track workflow lag between encounter close and charge entry to maintain days in receivables outstanding at or below 30 days.
3. Claims and Billing
Standardize claim build by payer to format, attachment, and timing rules. Scrubber and get to 98.4 percent clean claims.
Automate statements, ERA posting, and secondary claims. Monitor claim status and contact all open claims by day 21. Most payers will answer within that timeframe.
Anticipate 5 to 10 percent early denial rates, and work rejections the same day to prevent aging. Avoid the drain of preventable denials and appeals. Health systems in 2022 spent approximately $19.7 billion attempting to overturn denials.
4. Post-Service Resolution
Provide e-statements, card-on-file, wallets, and payment plans to stabilize cash flow and reduce bad debt. Keep data accessible and secure to fortify the mid-cycle and increase confidence.
Address billing inquiries quickly and in simple language. Neat, friendly responses stop conflicts and accelerate payments.
5. Analysis and Iteration
Watch core KPIs: first-pass resolution, denial rate by reason, DRO, clean claim rate, coding productivity, and underpayment yield.
Audit charts, codes, and payer contracts to identify revenue leaks and compliance risk. Leverage analytics to project cash and identify bottlenecks.
Close the loop with monthly reviews and ownership of fixes. Concentrate on process drivers to eliminate voids and increase throughput.
The Unseen Benefits
Optimization silently transforms the healthcare revenue cycle, enhancing the flow of care, cash, and compliance. More than quick, convenient payments, it creates a more reliable infrastructure upon which healthcare providers can depend.
- Clear prices cut through confusion, empower informed decisions, and increase price trust.
- Easy scheduling and simple registration halt downstream hazards before they spread.
- Automation reduces manual processing. Insurance claims submission, payment posting, and denial management are streamlined.
- Less claim denials increase yield and allow staff to address root causes.
- Cleaner data makes for better reporting, audits, and decisions across sites and service lines.
- Robust payer relationships abbreviate battles, accelerate determinations, and enhance clarification of policies.
- Equity feels better when billing rules are transparent and payment plans are fair.
Patient Experience
Transparent estimates, detailed statements and simple explanations assist patients in navigating care and expenses. Clear financial guidance engenders confidence in high-deductible or mixed coverage folks.
Fewer surprises through eligibility checks, real-time benefits verification, and price ranges that mirror contracted rates. That puts the kibosh on sticker shock and last-minute arguments.
Online portals and mobile pay options reduce friction. Digital reminders, multilingual support, and easy refunds make it feel human.
When the money side ticks down easily, they come back, do follow up and recommend the org. Enhanced patient involvement expands as they view expenses, options and schedules upfront.
Staff Morale
Simplified work saves you from burnout. When roles are clear, workflows are standard, and edits are guided in registration, coding, and billing, rework shrinks.
Automation tackles batch work, including claims submissions, remits posting, and first-pass denial routing, so your teams can actually spend their time fixing things that matter.
Regular KPI reviews, such as clean claim rate, first-pass yield, days in A/R, and denial rate, transform daily toil into tangible victories. Training associated with those KPIs gets better and faster.
Speedier resolution translates to fewer irate calls, fewer lines, and less weekend catch-up. Celebrating find-and-fix victories in huddles and disseminating playbooks between sites creates pride and retention.
Data Integrity
Accurate data at intake sets the tone: verified demographics, coverage, authorizations, and referral details that match the clinical record.
Front end edits keep miscoded modifiers, missing units, or stale payer IDs from getting through. Uniformity across systems enables consistent analytics and audit trails.
Privacy laws are in effect. Secure data with role-based access, encryption, and retention rules that comply with HIPAA (US) and equivalent privacy frameworks globally.
Payer Relations
Be aware of each payer’s modifications, schedules, and prior auth regulations. Filing non-fraudulent, clean, on-time claims that match contract terms establishes the foundation of trust.
Analyze work denials by type and root cause, not ticket by ticket. A hard-hitting appeal pack, including clinical notes, coding logic, and policy cites, accelerates turnarounds and increases reimbursement.
Apply contract analytics to identify underpayments, help renegotiate terms and monitor policy changes. Transparent, planned check-ins keep problems out in the open and minimize days in accounts receivable, increasing income security.
Technology’s Role
Digital tools lie at the heart of healthcare revenue cycle management. They connect patient access, coding, billing, and finance, ensuring that patient information remains accurate, secure, and accessible when needed. Powerful interoperability across EHR, billing, and online scheduling systems reduces rework, keeps records current, and enables real-time claim tracking, accelerating cash flow and enhancing revenue optimization.
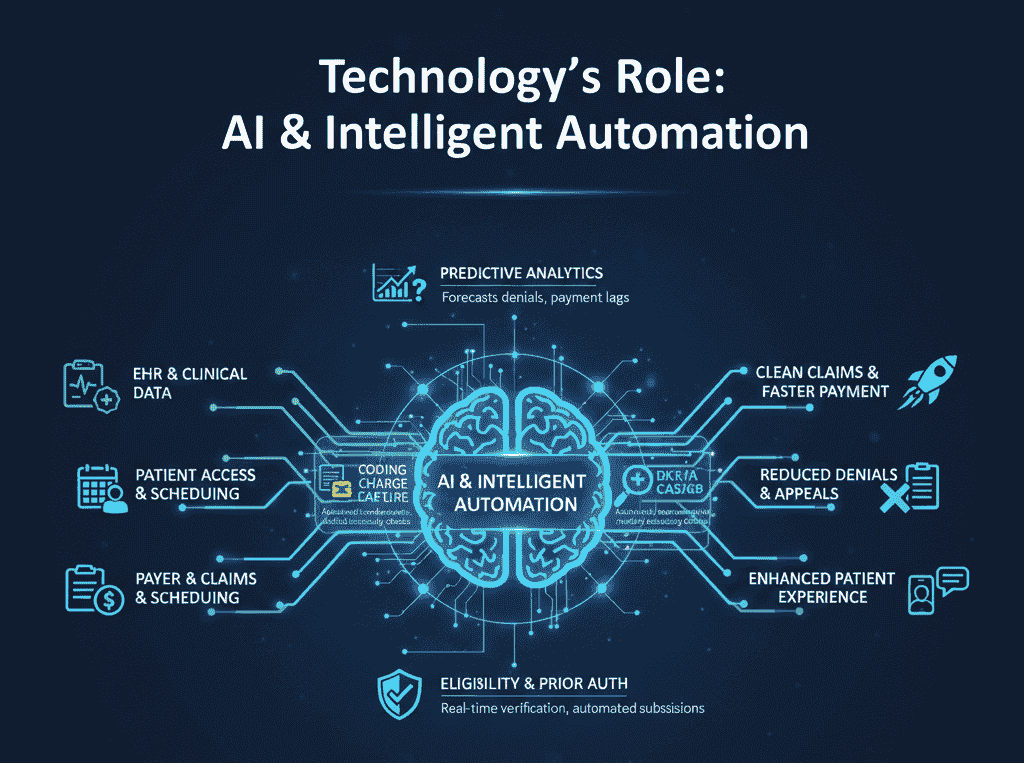
Automation
Automated eligibility checks verify coverage within seconds, eliminate front-desk back-and-forth, and avoid downstream denials. Technology’s Part: Tools submit clean claims, post remits, and reconcile payments without manual keying. Consider clearinghouse rules, electronic transaction toolkits, and auto-matching of EOB to ledger.
Rule-based edits halt common coding and charge mistakes prior to submission. For instance, prompts for missing modifiers, prior authorization, or documentation close gaps that cause delays.
By removing mundane work, teams can redirect hours to complex cases, payer outreach, and patient care. Volume spikes become simpler to manage without new headcount since queues scale with software, not shifts.
Real-time claim status feeds notify staff of rejections within minutes, not days. Quick fixes reduce aging and increase cash visibility.
Artificial Intelligence
AI goes further than rules, learning from patterns across claims, payers, and service lines. Models scan submissions to detect red flags, such as diagnosis-to-procedure pairings that don’t match or abnormal units that frequently cause denials.
They anticipate which claims are going to bounce, surface the precise remedy, and direct them to the appropriate individual prior to leaving. For coding and charge capture, recommendation engines identify missed charges, recommend particular codes from clinical text, and verify medical necessity with payer policies.
During denial management, bots put together appeal packets, draft letters with necessary citations, and select the optimal appeals route per payer. Insights on payer behavior, including turnaround times, common edits, and contract underpayments, feed dashboards that guide negotiations and worklists.
All of this minimizes mistakes, increases first-pass yield, and decreases days in accounts receivable while maintaining compliance and audit trails that hold up to scrutiny.
Predictive Analytics
Cash is predicted by predictive models that examine historic seasonality, real-time claim inventories, payer mix, and contract terms. Leaders can view next month’s cash range, the potential impact of a new clinic or code set, and anticipated payer delays.
These same tools spotlight at-risk claims and accounts, prioritize them by collectability, and initiate self-pay outreach plans before balances become aged. Capacity planning helps.
Technology’s role in patient volume by hour and service line forecasts direct staffing, slot templates, and pre-auth workload. These insights guide strategy, budget, and reporting for boards and regulators.
Overcoming Common Bottlenecks
The healthcare revenue cycle stumbles when information is fragmented, and processes remain manual, causing healthcare providers to respond too late. The remedy is to link systems, eliminate rework, and transition from fire-fighting to calm, proactive control, ensuring efficient revenue cycle management solutions.
Data Silos
Seamless integration with EHR, billing, clearinghouse, and scheduling ensures data flows cleanly from check-in to payment, enhancing the healthcare revenue cycle. A shared data model and one MPI put an end to mismatched records, which is essential for healthcare providers. Consolidating patient and financial data in one place allows for consolidated reporting on authorizations, denials, and aging without manual merges, optimizing revenue generation.
Eliminate duplicate entry at registration, coding, and payment posting to streamline the billing process. Minor mismatches such as payer ID, date format, or referral number trigger claim edits and delay cash. Mapping fields, locking needed information, and validating at the source are crucial steps.
Enhance cross-team flow by conducting weekly standups with front office, clinical, coding, and billing teams. This collaboration helps surface late dictation or missing operative reports, ensuring efficient revenue cycle management solutions.
Manual Processes
Paper, spreadsheets, and ad-hoc emails introduce latency and mistakes. Switch to digital intake, EHRs, and claims workqueue that routes by priority. Standardize steps for charge capture, coding, and claim edits.
Then automate repeats such as eligibility checks, coverage discovery, and claim status pulls. Make it even easier by using templates and computer-assisted coding to reduce variance and prompt missing documents to prevent late or missing dictation from holding up claims.
For prior authorizations, track 21 days from request, flag gaps on day 3, and submit missing items within 48 hours. When forms correspond to payer requirements and codes match insurance—HCPCS or generic where applicable—approval rates increase and rework decreases.
Technology liberates humans to address edge cases, sophisticated coding, or patient inquiries. That shift helps with staffing shortages by shifting effort from data entry to higher-value work. Maintain strict standards on documentation quality, as thorough notes and accurate coding continue to be the foundation for clean claims and maximum reimbursement.
Reactive Management
Shift from ‘repair post denial’ to early identification within the healthcare revenue cycle. Establish real-time dashboards for first-pass yield, denial rate by reason code, and documentation lag to optimize revenue cycle management solutions. Alerts should trigger when a claim lingers or when a payer changes a rule, facilitating efficient revenue cycle practices.
Deny claims the day they arrive and categorize root causes—such as lost paperwork or code mismatch—to enhance patient financing programs. Target workflow catalysts like charge-capture timing and bottlenecks caused by manual data entry to prevent revenue leakage instead of chasing it. This proactive approach aids in improving patient experiences and revenue generation.
Introduce daily check-ins and a short huddle to share one-page metrics, identify fixes, and record owners and due dates. This fosters a collaborative environment among healthcare providers and enhances overall revenue cycle performance.
Measuring True Success
These clear goals, shared definitions, and routine review determine if healthcare revenue cycle optimization truly works. By measuring what is important, connecting metrics to owners, and benchmarking results against industry ranges, healthcare providers can establish reasonable goals and steer change without guesswork.
Foundational Metrics
Monitor the fundamentals that reflect the well-being of billing, collections, and cash. These core KPIs establish your baseline and tone for accountability and improvement.
- Clean claims rate is the share of claims that pass edits and go out error free.
- First-pass resolution rate is the percentage of claims paid on first submission, which is a direct read on process quality.
- Denial rate is the portion of claims denied by payers. Usual rates are between 5 percent and 10 percent, and rates over 10 percent indicate serious problems.
- Days in A/R: average time to collect. Monitor the percent of A/R over 90 days to identify potential aging risk.
- Net collections ratio: cash collected versus expected shows real yield.
- Patient collections at point of service and post-visit to payment plans and digital tools.
- Missed charges: Recurring misses hint at workflow gaps or persistent, undisputed payer denials.
Track net revenue and cash flow on a consistent week-to-week basis. RCM costs frequently hover at 3% to 5% of all patient revenue. Trimming waste matters since inefficiencies cost providers billions annually.
Shoot for coding productivity at 95% or higher so that less than 5% of the work queues up. Increase first-pass resolution and clean claims rates; they will compound. Every 1% efficiency lift saves approximately USD 50,000 per year in rework.
Build a simple dashboard for revenue cycle leads: top KPIs, denial reasons, aging buckets, clean claims trend, first-pass rate, missed charges, coder backlog, and payer turnaround times.
Advanced Indicators
Beyond the baseline, track cost-to-collect, staff productivity, and the patient’s billing experience. Contrast teams and locations to identify variance.
For example, higher call handle time and low dispute resolution typically indicate nebulous statements. Tie insights to root causes with analytics: which CPT codes, payers, or clinics drive denials, write-offs, long A/R, or refunds.
Use audit trails to identify process breaks such as eligibility misses, coding drift, or front-desk capture errors and pilot automation where it shrinks repetitive work. Many providers experience denial rates drop within months of targeted automation.
| Indicator | What it shows | Example benchmark | Action if off-track |
| Cost-to-collect | Expense per 1 unit of cash | Trend down quarter over quarter | Automate edits; rebalance staffing |
| Staff productivity | Claims/coder/day; calls resolved/agent/day | Coding >95% queue clear | Cross-train; standardize work |
| Patient billing satisfaction | NPS/CSAT for billing touchpoints | Above service line median | Simplify statements; add self‑pay plans |
| Root-cause denial map | Top codes/payers/error types | Denial rate 5%–10% | Fix front-end checks; update rules |
Predictive KPIs
By measuring real accomplishment and forecasted accomplishment, construct models that predict probable denials, payment lags, and patient non-payments by combining signals from eligibility, benefits, code trends, past payer conduct, and socio-economic indicators.
Project net revenue by payer and service line while leveraging existing authorization queues, scheduled volume, and historical turnaround. Integrate this into a 90-day cash forecast with confidence intervals.
Set thresholds such as a projected denial spike above 9 percent, accounts receivable over 90 days rising by 2 percentage points, or payer lag exceeding 7 days to trigger playbooks: pre-bill audits, targeted coder reviews, or payer outreach.
Feed predictive KPIs into executive dashboards so leaders see risk early, align resources fast, and benchmark against industry ranges to set realistic goals and track whether actions cut denials to less than 10 percent, hold coding productivity above 95 percent, and keep clean claims and first-pass rates climbing.
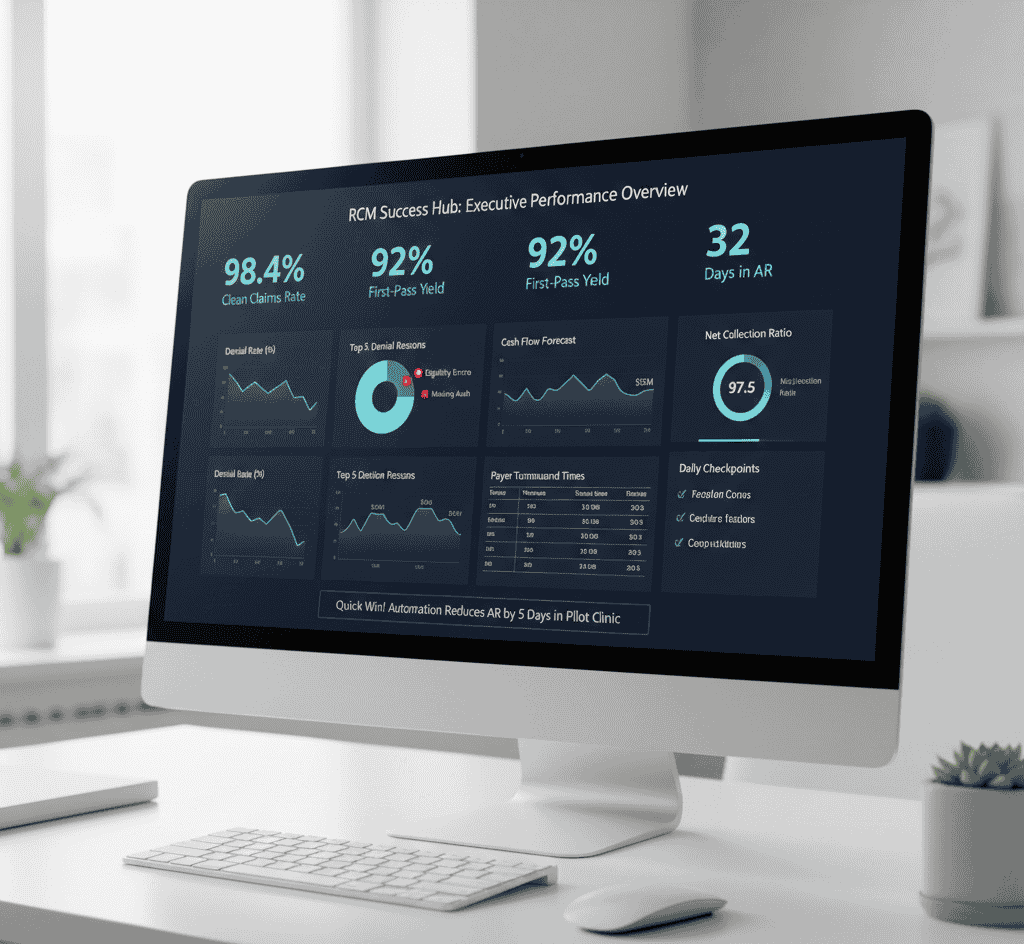
Conclusion
RCM wins begin with well-defined measures and consistent audits. Even the best revenue cycle management optimization teams that fix front desk data, code fast and follow up on claims see cash move faster. Technology gets us started but it’s the people who make it stay. Think small wins that stack. Reduce denials by 15%. Drive clean claim rate to 95%. Aim to post charges in less than 24 hours. Close old A/R in 30 days. Every step puts cash on the bottom line and cuts back on stress.
Real examples guide the way. A clinic established a daily huddle and reduced rework by 50%. A lab established payer guidelines and increased first pass pay. A hospital used alerts and stopped late authorizations.
To secure advances, establish three goals, select a strategy, and monitor the following 90 days. Want a fast schedule for your store. Schedule a brief audit and begin next week.
Frequently Asked Questions
What is revenue cycle management (RCM) optimization?
RCM optimization, or healthcare revenue cycle optimization, is the ongoing refinement of financial touch points from patient access to reconciliation. It aligns people, processes, and technology to reduce denials, speed cash flow, cut costs, and improve patient experiences in healthcare organizations.
How can we quickly improve our revenue cycle?
Begin with eligibility, coding, and denial prevention in the healthcare revenue cycle. Standardize charge capture and implement real-time claim scrubbing. Monitor daily with dashboards to optimize revenue cycle performance. Educate staff on root-cause denials and automate routine tasks to enhance billing processes. These actions increase first-pass yield and decrease days in accounts receivable.
What unseen benefits come from RCM optimization?
Improving cash flow is a no brainer for healthcare providers. Unseen gains include less write-offs, better patient satisfaction, and enhanced compliance, all contributing to an efficient revenue cycle. Quality data enables smarter contracts and informed service-line decisions, ultimately reducing burnout by minimizing rework and firefighting.
How does technology strengthen RCM performance?
Utilize healthcare revenue cycle analytics to identify revenue leakage effectively. Deploy automation for eligibility checks and claim edits, while combining coding support and denial forecasting. Providing digital payments and patient estimates enhances decision-making and streamlines the entire revenue cycle.
What common bottlenecks should we fix first?
Key bottlenecks in the healthcare revenue cycle include incomplete patient registrations, missing authorizations, charge lag, coding backlogs, and poor denial follow-up. To enhance revenue cycle management solutions, focus on data quality at intake, authorization automation, and enforcing charge capture timelines.
How do we measure true success in RCM?
Monitor first pass claim rates and denial rates by category while tracking days in A/R and net collection rates to optimize the healthcare revenue cycle. Utilize trend lines and benchmarks to connect targets to service lines and payer mix for improved patient financing and efficient revenue cycle management.
How long until we see measurable ROI?
Quick wins in the healthcare revenue cycle can show up in 60 to 90 days through claim edits, eligibility checks, and denial prevention. More significant improvements in revenue cycle management solutions require 6 to 12 months through workflow redesign and system integrations.







