Introduction
Outsource medical billing services allows U.S. healthcare providers to delegate complex billing tasks to specialized revenue cycle experts. These teams manage coding, claim submission, payment posting, denial management, and reporting, freeing clinics and hospitals from daily administrative burdens.
Many practices face persistent billing challenges, including claim denials due to coding errors, extended accounts receivable (AR) cycles that slow cash flow, staffing shortages that disrupt workflows, and compliance risks from HIPAA or ICD-10 updates.
Across the United States, small clinics, multi-specialty groups, and large hospitals are turning to outsourced medical billing to streamline revenue cycles, reduce costs, and focus on patient care. With faster reimbursements, fewer denials, and lower overhead, outsourcing boosts revenue while improving operational efficiency, making it an essential strategy for modern healthcare providers.
What Is Outsourced Medical Billing?
Clear Definition
Outsourced medical billing is the process of hiring an external, specialized team to handle your healthcare practice’s billing and revenue cycle management. This includes coding patient visits, submitting claims to insurance payers, posting payments, managing denials, and providing detailed financial reports. Essentially, it shifts the responsibility of revenue collection from your in-house staff to trained experts who focus solely on optimizing billing processes.
How It Differs from In-House Billing
Unlike in-house billing, where your staff handles all claims, follow-ups, and reporting, outsourcing provides:
- Specialized Expertise: Certified coders and billing professionals manage complex codes and payer-specific rules.
- Advanced Technology: Outsourcing partners often use automated platforms with rules engines, dashboards, and analytics for faster, more accurate claims processing.
- Scalable Support: Outsourced teams can handle fluctuating claim volumes, seasonal peaks, and multi-specialty billing without adding internal headcount.
- Reduced Administrative Burden: Your staff spends less time on billing tasks and more on patient care.
In contrast, in-house billing often requires significant investment in staff, software, training, and compliance management. Mistakes or delays in coding, claim submission, or denial handling can directly impact revenue and cash flow.
Who Should Consider Outsourcing
Outsourced medical billing is ideal for:
- Small to Medium Practices: Clinics without dedicated billing departments benefit from cost savings and expertise.
- Multi-Specialty Clinics: Providers with diverse specialties, such as Cardiology, Pediatrics, or Mental Health, need accurate, payer-specific coding.
- High-Volume Practices: Hospitals or large groups with many claims require faster turnaround and denial prevention.
- Practices Facing Staff Shortages: Outsourcing removes dependency on hiring and training internal billing staff.
- Providers Seeking Compliance Assurance: Billing partners stay updated on HIPAA regulations, ICD-10 changes, and payer policy updates.
By outsourcing medical billing, these providers can increase revenue, reduce errors, and free up staff time, allowing them to focus on what matters most: delivering high-quality patient care.
What Services Are Included in Outsourced Medical Billing?
Outsourced medical billing covers a wide range of services designed to streamline the revenue cycle, reduce errors, and ensure timely payments. Healthcare providers in the U.S. can rely on professional billing teams to handle every step of the process, from coding to compliance.
Medical Billing and Coding (ICD-10, CPT, HCPCS)
Certified coders review patient encounters and assign accurate ICD-10, CPT, and HCPCS codes. Proper coding ensures claims are submitted correctly the first time, reducing denials and delays in payment. Outsourcing provides access to coding expertise that keeps up with the latest industry updates and payer-specific rules.
Accounts Receivable (AR) and Denial Management
Outsourced billing teams manage AR by tracking unpaid claims, following up with payers, and appealing denied claims. By reducing denial rates and shortening AR cycles, practices experience faster cash flow and fewer write-offs. Real-time reporting allows providers to monitor collections and identify trends in denials.
Insurance Verification
Before a patient’s visit, billing specialists verify insurance coverage to confirm eligibility and benefits. Accurate verification prevents claim rejections due to incorrect or missing information and helps patients understand their financial responsibility upfront.
Prior Authorizations
Many procedures and treatments require prior authorization from insurance providers. Outsourced billing teams handle the authorization process, submitting documentation to payers, and ensuring approvals are obtained before services are provided. This reduces delays in patient care and billing rejections.
Provider Credentialing Support
Credentialing is essential for providers to be recognized by insurance payers. Billing partners assist with enrollment, renewals, and documentation management, ensuring your practice can bill efficiently and remain compliant with payer requirements.
Revenue Cycle Management (RCM)
Full-service outsourced billing integrates all revenue cycle management functions, including charge capture, claims submission, payment posting, denial management, and reporting. RCM solutions provide end-to-end visibility and optimize financial performance across your practice or hospital.
Billing and Coding Audits
Outsourcing includes periodic audits to review coding accuracy, compliance, and documentation. Audits identify potential errors, prevent claim denials, and improve overall revenue integrity. Providers gain insights into workflow improvements and staff training needs.
HIPAA Compliance Support
Billing partners maintain HIPAA-compliant workflows, secure data storage, and encrypted communication to protect patient information. Regular security audits and adherence to federal regulations ensure your practice avoids costly penalties and maintains trust with patients.
Why Do Healthcare Providers Outsource Medical Billing Services?
Outsourcing medical billing offers healthcare providers a way to streamline operations, reduce errors, and improve financial performance. By partnering with specialized billing teams, practices can focus on patient care while ensuring their revenue cycle is handled efficiently.
Reduce Operational Costs
Managing an in-house billing team can be expensive. Salaries, benefits, software licenses, training, and IT infrastructure all add up. Outsourcing eliminates these overhead costs, allowing practices to pay a predictable fee based on collections or claims. This model reduces administrative expenses while still providing access to experienced billing professionals.
Increase Clean Claim Rate
Accurate coding and claim submission are critical to timely reimbursement. Outsourced billing teams use certified coders, automated claim scrubbing, and payer-specific rules to maximize first-pass claim acceptance. Higher clean claim rates mean fewer rejections and faster payments, improving overall practice revenue.
Improve Cash Flow & Reduce AR Days
Delayed payments can disrupt a clinic’s cash flow. Billing specialists track accounts receivable, follow up with payers promptly, and appeal denials efficiently. Practices often see a reduction in AR days, allowing for faster revenue collection and more predictable cash flow for payroll, operations, and growth initiatives.
Minimize Claim Denials
Denied claims are one of the biggest revenue drains for healthcare providers. Outsourced teams proactively manage denials by identifying recurring coding errors, verifying payer requirements, and submitting appeals with proper documentation. This prevents repeated mistakes and protects practice revenue.
Ensure HIPAA Compliance
Compliance with HIPAA and other federal regulations is non-negotiable. Professional billing partners maintain encrypted data transmission, secure storage, role-based access, and audit trails. This reduces risk of breaches, penalties, and regulatory issues, keeping patient information safe and your practice compliant.
Scale for Growth & Multi-Specialty Practices
Outsourced medical billing is highly scalable. Whether a practice adds new locations, expands services, or introduces telehealth programs, billing partners can adjust resources quickly without requiring new staff or software investments. Multi-specialty clinics, including Cardiology, Pediatrics, Mental Health, and OBGYN, benefit from payer-specific expertise and tailored workflows that support diverse service lines.
How Does Medical Billing Outsourcing Work?
Outsourced medical billing streamlines the revenue cycle by delegating key billing tasks to specialized experts. This process ensures accurate coding, faster claim submissions, and improved cash flow for U.S. healthcare providers. Here’s how it works step by step:
Step 1 – Patient Data & Charge Capture
The process begins with collecting patient demographics, insurance information, and encounter notes from your practice. Billing specialists capture charges for every service provided, ensuring that all billable procedures are documented accurately. This step lays the foundation for clean claims and reduces the risk of errors.
Step 2 – Coding Review & Claim Scrubbing
Certified coders review the captured charges and apply appropriate ICD-10, CPT, and HCPCS codes. Automated claim-scrubbing tools detect potential errors, missing information, or payer-specific issues before submission. Accurate coding minimizes denials and ensures compliance with industry standards.
Step 3 – Electronic Claim Submission
Once claims are verified, the billing team submits them electronically to insurance payers using secure channels. Electronic submissions accelerate processing, reduce delays, and provide real-time confirmation of receipt. This ensures claims reach payers quickly and efficiently.
Step 4 – Payment Posting & Reconciliation
Payments received from insurance companies and patients are posted to the practice’s system. The billing team reconciles payments against submitted claims, identifies discrepancies, and ensures accurate accounting. Proper reconciliation improves financial visibility and prevents revenue leakage.
Step 5 – Denial Management & Appeals
Denied claims are tracked, analyzed, and corrected promptly. Billing specialists identify the reason for denials, submit appeals with supporting documentation, and work with payers to resolve issues. This proactive approach reduces revenue loss and increases overall collection rates.
Step 6 – Reporting & Performance Analytics
Outsourced billing partners provide detailed reports and dashboards that track key performance indicators (KPIs), including clean claim rates, denial trends, AR days, and net collections. These insights allow practices to monitor financial performance, identify opportunities for improvement, and make data-driven decisions to optimize revenue cycles.
How Much Does It Cost to Outsource Medical Billing?
Understanding the cost of outsourcing medical billing is essential for U.S. healthcare providers looking to improve cash flow and reduce operational expenses. Pricing varies depending on practice size, specialty, claim volume, and service scope.
Percentage-Based Pricing (3%–8%)
Many billing companies charge a percentage of monthly collections, typically ranging from 4% to 10%. This model aligns the billing partner’s incentives with your revenue goals: the more they collect efficiently, the better your practice benefits. Percentage-based pricing works well for high-volume practices seeking predictable costs tied directly to revenue.
Per-Claim Pricing
Some providers prefer per-claim billing, where the practice pays a fixed fee for each processed claim. This model is ideal for smaller clinics or low-volume practices, offering predictable costs per transaction while still benefiting from expert billing support.
Hybrid Pricing Models
Hybrid pricing combines a base fee with variable charges tied to claim volume, complexity, or specific services. This flexible approach allows practices to scale costs according to their needs while maintaining access to advanced billing services.
Factors That Affect Cost
Several factors influence outsourced medical billing costs:
- Specialty: High-complexity specialties like Cardiology, Oncology, or Mental Health may require more experienced coders and longer claim processing.
- Volume: Practices with more patient visits or claims will incur higher fees under per-claim or percentage-based models.
- Payer Mix: Multiple insurance payers with different rules increase administrative complexity, impacting pricing.
- Service Scope: Full-service billing (including AR follow-up, prior authorizations, and denial management) costs more than basic claim submission.
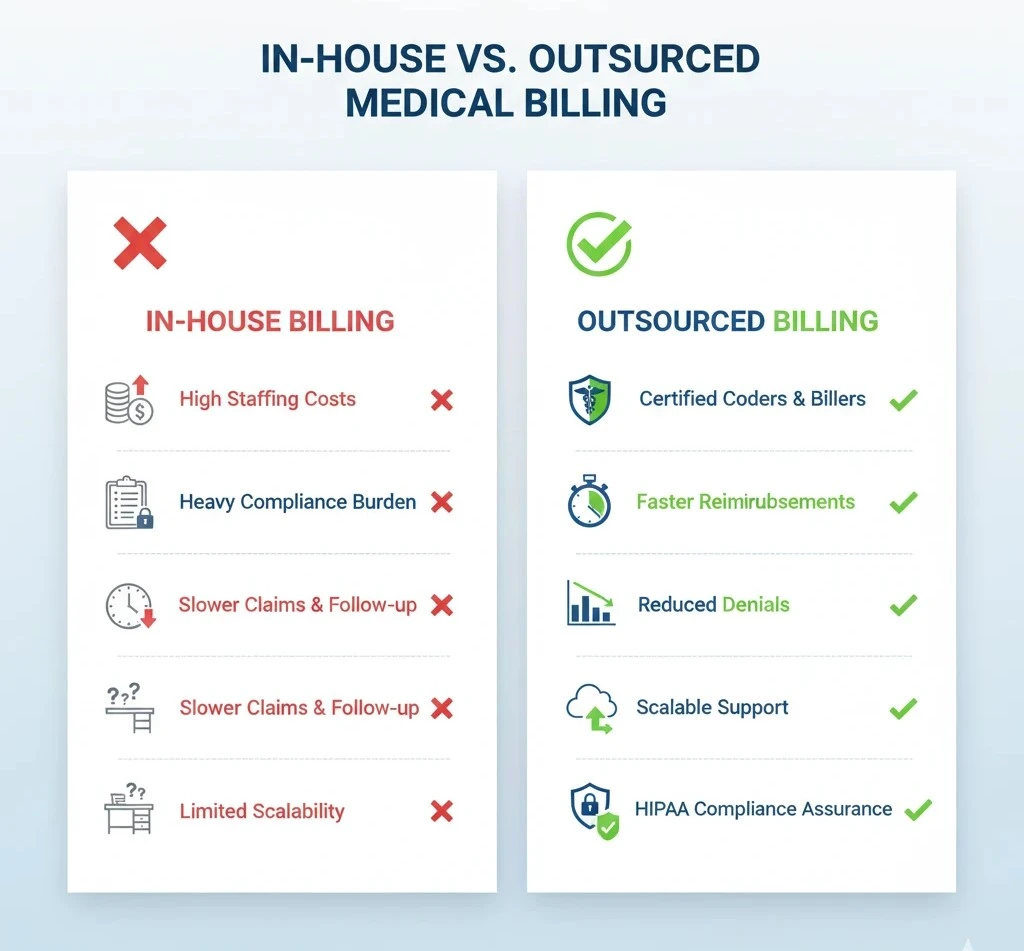
ROI Comparison: In-House vs Outsourced Billing
Outsourcing can provide a significant return on investment:
- Lower Labor Costs: No need to hire, train, or retain in-house billing staff.
- Faster Reimbursements: Reduced AR days and higher first-pass claim rates accelerate cash flow.
- Reduced Denials: Expert coding and denial management prevent revenue leakage.
- Predictable Expenses: Fixed or percentage-based fees simplify budgeting and reduce unexpected overhead.
Compared to maintaining an in-house billing team, outsourcing often saves 20%–40% of operational costs while improving collections and practice efficiency.
What Results Can You Expect in the First 90 Days?
Outsourcing medical billing often delivers noticeable improvements in financial performance and operational efficiency within the first three months. Here’s what U.S. healthcare providers can typically expect:
Clean Claim Rate Improvement
A primary benefit of outsourcing is a higher first-pass clean claim rate. Professional billing teams use certified coders, automated claim-scrubbing tools, and payer-specific rules to ensure claims are accurate before submission. Practices often see first-pass rates increase to 95% or higher, reducing rework and speeding up reimbursements.
Denial Reduction Percentage
Denied claims are a major source of lost revenue. Outsourced billing partners proactively manage denials by analyzing trends, correcting errors, and submitting timely appeals. Many practices experience a 10–20% reduction in claim denials within the first 90 days.
AR Days Reduction
Accounts receivable (AR) days measure how long it takes to collect payments. Outsourced teams track unpaid claims, follow up with payers, and streamline payment posting. This typically results in shorter AR cycles, improving cash flow and reducing financial stress for the practice.
Increased Net Collection Rate
By minimizing errors, preventing denials, and ensuring timely follow-ups, outsourcing can increase net collections. Practices often see measurable revenue growth, allowing better budgeting, payroll management, and investment in patient care services.
Improved Reporting Transparency
Outsourced billing partners provide clear, detailed dashboards and performance reports. Practices gain real-time visibility into claims, denials, AR trends, and KPIs, enabling informed decision-making and better oversight of financial performance.
Is Outsourcing Medical Billing Right for Your Practice?
Outsourced medical billing is not a one-size-fits-all solution. The right fit depends on your practice size, specialty, patient volume, and operational needs. Here’s who benefits the most:
Small Practices
Small clinics with limited staff often struggle to manage billing internally. Outsourcing allows them to access expert coders, denial management, and AR follow-up without hiring full-time employees. This reduces overhead while improving cash flow and claim accuracy.
Large Clinics
Large healthcare facilities or hospital-affiliated clinics generate high claim volumes that can overwhelm in-house teams. Outsourced billing provides scalable support, ensuring timely submission, payment posting, and denial management for hundreds or thousands of claims per month.
Multi-Specialty Groups
Practices offering multiple specialties, such as Cardiology, Orthopedics, and Pediatrics, face complex coding and payer requirements. Professional billing partners handle specialty-specific rules and workflows, reducing errors and optimizing reimbursement across all service lines.
Telehealth Providers
Telemedicine services present unique billing challenges, including remote service coding and payer requirements. Outsourced billing teams experienced in telehealth ensure accurate claim submission, prior authorizations, and AR management, helping providers maintain compliance and revenue flow.
Specialty-Specific Needs (Cardiology, Mental Health, OBGYN, etc.)
Different specialties have different billing requirements, from complex procedures in Cardiology to mental health therapy sessions or OB/GYN prenatal care. Outsourced billing companies provide certified coders familiar with each specialty, minimizing denials and maximizing reimbursements.
How to Choose the Best Medical Billing Company
Selecting the right outsourced medical billing partner is critical to improving revenue, reducing denials, and maintaining compliance. Here are the key factors U.S. healthcare providers should consider:
Certified Coders (AAPC, AHIMA)
Ensure the billing company employs certified coders with credentials like AAPC (CPC) or AHIMA (CCS). Certified coders understand complex coding standards, updates, and payer-specific rules, which reduces denials and improves first-pass claim rates.
Denial Management Expertise
A strong billing partner proactively manages claim denials, appeals, and payer follow-ups. Ask about their success rate in overturning denials, tracking recurring errors, and implementing corrective measures to prevent revenue loss.
Technology & EHR Integration
Look for billing companies that use advanced billing software with automation, claim scrubbing, and analytics. Seamless integration with your EHR or practice management system ensures accurate data transfer, reduces manual entry errors, and provides real-time dashboards for performance monitoring.
Transparent Pricing
Your billing partner should offer clear pricing models—percentage of collections, per-claim, or hybrid—without hidden fees. Transparency ensures predictable costs and lets you evaluate ROI effectively.
HIPAA & Data Security Standards
Security and compliance are non-negotiable. Verify that your billing partner maintains HIPAA-compliant workflows, encrypted data storage, role-based access, and routine security audits. This protects patient data and reduces regulatory risk.
Reporting & KPIs (First-Pass Rate, AR Days)
Choose a partner that provides comprehensive reporting with key metrics such as first-pass claim rate, denial trends, AR days, and net collection rate. Regular dashboards allow you to track performance, identify issues early, and make data-driven decisions to optimize your revenue cycle.
Common Risks of Outsourcing Medical Billing (And How to Avoid Them)
While outsourcing medical billing can bring significant benefits, it also introduces potential risks that healthcare providers must manage. Awareness and proactive strategies can help practices mitigate these risks.
Data Security Concerns
Patient data is highly sensitive and protected under HIPAA. Outsourcing introduces risks if a partner lacks proper security protocols. How to avoid:
- Choose a partner with HIPAA-compliant systems, encryption for data in transit and at rest, and regular third-party security audits.
- Verify role-based access controls and audit logs to ensure proper data handling.
Communication Gaps
Misunderstandings between your practice and the billing company can lead to delayed claims, untracked denials, or overlooked payments. How to avoid:
- Establish clear communication channels, scheduled status calls, and shared dashboards.
- Define escalation protocols for urgent issues and ensure both teams have point-of-contact owners.
Hidden Fees
Some billing providers may charge extra for add-on services, software access, or claim corrections. How to avoid:
- Request transparent pricing upfront, including per-claim fees, percentage-based rates, or hybrid models.
- Include clear terms in the contract for additional services or volume surcharges.
Loss of Control
Outsourcing means handing over operational tasks, which can feel like a loss of oversight. How to avoid:
- Maintain visibility through real-time dashboards, monthly performance reports, and KPIs.
- Define roles and responsibilities clearly using a RACI chart (Responsible, Accountable, Consulted, Informed) for billing processes.
Poor Onboarding
A rushed or poorly planned transition can cause errors, delays, or compliance issues. How to avoid:
- Develop a structured 30–60–90 day onboarding plan with milestones and responsibilities.
- Include staff training, secure data migration, and parallel processing to ensure a smooth handover.
Final Thoughts
Outsourcing medical billing services is a proven strategy for U.S. healthcare providers to reduce operational costs, improve cash flow, and minimize claim denials. By partnering with experienced billing experts, practices can ensure accurate coding, faster reimbursements, HIPAA compliance, and scalable support for multi-specialty clinics and telehealth providers. With clear reporting, KPIs, and dedicated support, outsourcing allows clinicians to focus on patient care while optimizing revenue.
Take Action Today: Identify your top billing challenges and connect with a trusted medical billing partner to streamline your revenue cycle, boost collections, and cut administrative costs.