Medical billing trends in 2026 are being shaped by new healthcare regulations, evolving payer policies, staffing shortages, and increased use of automation in revenue cycle management (RCM). For small practices, multi-specialty groups, and hospitals across the United States, these changes directly impact reimbursement rates, claim approvals, compliance risk, and overall cash flow.
Understanding the latest medical billing industry trends is essential for healthcare providers who want to reduce denials, improve collections, and maintain financial stability in a rapidly changing reimbursement environment.
Here are the most important medical billing industry trends in 2026 and what they mean for your organization.
Table of Contents
1. Automation Is No Longer Optional, But Oversight Still Matters
Automation tools, AI-assisted coding, and intelligent claim scrubbing systems are becoming standard across the industry. From eligibility verification to denial prediction, advanced systems now help billing teams work faster and reduce manual errors.
However, automation is not a replacement for expertise.
In 2026, successful healthcare organizations are combining:
- Automated claim scrubbing
- Real-time eligibility checks
- AI-supported coding assistance
- Human review by certified billing professionals
The practices seeing the best results are those using technology to improve clean claim rates while maintaining strong compliance oversight.
2. Denial Management Is Becoming More Complex
Payer policies continue to evolve. Pre-authorization requirements are increasing, documentation standards are tightening, and coding specificity demands are growing.
Denials are no longer just administrative issues — they are revenue threats.
Key trends in denial management include:
- Increased scrutiny of medical necessity documentation
- Stricter modifiers and bundling edits
- Higher denial rates for telehealth and specialty services
- More aggressive audits
Healthcare providers who proactively track denial trends, appeal quickly, and analyze root causes are significantly improving collections.

3. Regulatory Compliance in Medical Billing Is More Critical Than Ever in 2026
Regulatory compliance remains one of the most important priorities in medical billing and revenue cycle management (RCM) in 2026. As federal oversight increases and reimbursement rules become more complex, healthcare providers must ensure their billing processes meet current compliance standards to avoid revenue disruption.
Billing departments must stay aligned with regulations and guidance from:
- Centers for Medicare & Medicaid Services (CMS)
- Office for Civil Rights (OCR)
- U.S. Department of Health & Human Services (HHS)
In addition to strict HIPAA enforcement, providers must navigate evolving reimbursement policies, price transparency requirements, audit activity, and value-based care reporting standards. Even minor documentation or coding errors can trigger denials, recoupments, or compliance investigations.
Failure to maintain billing compliance can result in:
- Delayed reimbursements
- Increased payer audits
- Financial penalties
- Legal exposure
- Reputational damage
In 2026, proactive compliance monitoring, internal audits, accurate coding practices, and updated billing workflows are essential components of a strong revenue cycle strategy. Healthcare organizations that prioritize regulatory compliance protect both their revenue and their long-term operational stability.
4. Labor Shortages Are Driving Outsourcing Growth
Staffing challenges continue to impact in-house billing departments. Many practices report:
- Difficulty hiring experienced billers
- High turnover rates
- Training gaps
- Burnout within revenue cycle teams
As a result, outsourcing medical billing is becoming less of a cost-saving measure and more of a stability strategy.
Small practices benefit from:
- Reduced overhead
- Consistent claim follow-up
- Access to certified billing specialists
Hospitals and multi-specialty groups gain:
- Scalable support
- Advanced reporting
- Improved cash flow predictability
In 2026, outsourcing is increasingly viewed as a strategic partnership, and many healthcare providers rely on a trusted medical billing partner to ensure smooth revenue cycle management rather than treating it as just an operational decision.
5. Data-Driven Medical Billing KPIs Are Transforming Revenue Cycle Strategy in 2026
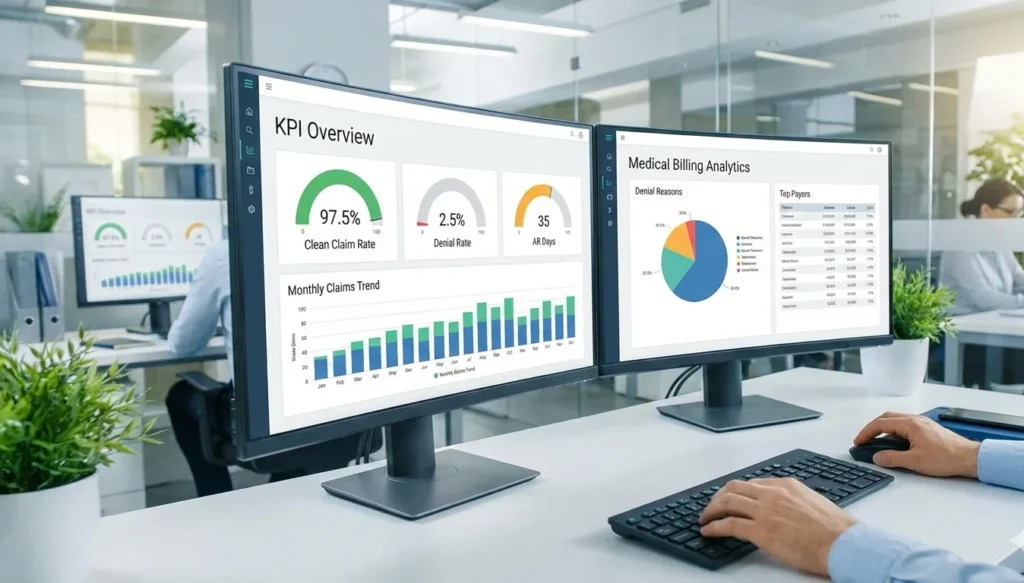
In 2026, successful healthcare organizations are using data-driven medical billing KPIs to strengthen revenue cycle management (RCM) and improve financial performance. Instead of reacting to cash flow problems after they occur, small practices, multi-specialty groups, and hospitals are leveraging real-time analytics to monitor billing performance and reduce revenue leakage.
The most important medical billing KPIs healthcare leaders are tracking include:
- Clean claim rate (percentage of claims paid without edits or denials)
- First-pass resolution rate
- Days in Accounts Receivable (AR)
- Net collection rate
- Denial rate by payer
These revenue cycle metrics provide clear insight into operational efficiency, payer behavior, and billing accuracy. When monitored consistently, they help identify hidden bottlenecks before they impact cash flow.
With advanced dashboards and performance reporting tools, healthcare organizations can:
- Detect payer-specific denial trends
- Identify coding and documentation gaps
- Reduce write-offs and underpayments
- Improve financial forecasting and budgeting accuracy
Data transparency is no longer optional in medical billing. In 2026, organizations that rely on measurable KPIs and actionable revenue cycle analytics are better positioned to increase collections, reduce AR days, and maintain predictable financial stability.
6. Telehealth and Specialty Billing Continue to Evolve
Telehealth adoption continues to grow, and specialty services—from cardiology to oncology—are seeing increased demand. However, reimbursement rules are constantly evolving, making accurate billing more important than ever for small practices, multi-specialty groups, and hospitals.
Key telehealth and specialty billing challenges in 2026 include:
- Modifier accuracy for proper claim adjudication
- Place-of-service coding updates reflecting virtual or hybrid visits
- Documentation alignment with payer requirements
- State-specific regulations impacting coverage and reimbursement
Ensuring precision in telehealth and specialty billing not only maximizes revenue but also reduces compliance risk and costly claim denials. Organizations that stay proactive with updated coding guidelines and training will maintain smooth revenue cycles and improve financial outcomes.
7. Value-Based Care Is Expanding
Fee-for-service reimbursement models are gradually being supplemented by value-based programs.
This shift requires billing systems to:
- Track quality metrics
- Align coding accuracy with patient outcomes
- Ensure proper documentation supports reimbursement
Organizations that integrate clinical documentation improvement (CDI) with billing processes are better positioned to maximize revenue under evolving payment models.
What These Trends Mean for Your Organization
Whether you operate a small private practice or manage a large hospital system, these trends share one common theme:
Revenue cycle management is becoming more strategic.
Medical billing is no longer just about submitting claims. It now requires:
- Regulatory expertise
- Advanced technology
- Denial analytics
- Compliance oversight
- Performance reporting
Organizations that adapt proactively will see:
- Faster reimbursements
- Lower denial rates
- Stronger compliance
- Improved cash flow
Those that delay modernization may face increased financial strain.
Struggling With Claim Denials or Slow Reimbursements?
Our medical billing experts help practices reduce denials, optimize revenue cycle management, and increase collections.
Final Thoughts
The medical billing industry in 2026 is defined by complexity, technology integration, and tighter regulatory oversight. For U.S. healthcare providers, staying informed about these changes is critical to maintaining financial health.
Small practices, multi-specialty groups, and hospitals that embrace strategic revenue cycle management, whether in-house or through experienced billing partners, are best positioned to thrive in the evolving reimbursement environment.
Take Control of Your Revenue Today: Partner with a trusted medical billing and coding specialist to reduce denials, streamline claims, and maximize reimbursements. Contact us now at +1 (302) 262 1168 or info@ebillient.com to schedule a free consultation and safeguard your practice’s financial future.
Frequently Asked Questions:
1. What are the biggest medical billing challenges in 2026 for U.S. healthcare providers?
The biggest challenges include stricter payer policies, rising claim denials, increased documentation requirements, labor shortages, and evolving telehealth and specialty billing rules. Providers must adopt automation, track KPIs, and ensure compliance to address these challenges effectively.
2. How does automation improve medical billing and revenue cycle management?
Automation reduces manual errors, speeds up claims processing, and improves clean claim rates. AI-assisted coding, claim scrubbing, and real-time eligibility checks help billing teams submit more accurate claims while allowing certified professionals to focus on complex cases.
3. Why is denial management more critical than ever in 2026?
Denial management is crucial because payers are applying stricter policies and auditing more aggressively. Tracking denial trends, appealing quickly, and addressing root causes can prevent revenue loss and improve overall cash flow for healthcare providers.
4. How can healthcare providers benefit from outsourcing medical billing?
Outsourcing provides access to experienced billing specialists, scalable support, consistent claim follow-up, and advanced reporting. It helps practices reduce overhead, improve collections, and manage staff shortages more efficiently.
5. What role do KPIs and data analytics play in modern medical billing?
KPIs like clean claim rate, denial rate, first-pass resolution rate, and days in accounts receivable allow providers to monitor revenue cycle performance. Data-driven insights help detect inefficiencies, prevent revenue leakage, and improve financial forecasting and cash flow.
Stay updated on medical billing trends, follow us on Facebook







